Rehab Articles
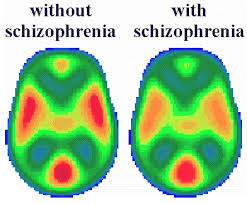
Brain imaging holds the key to why healthy siblings of schizophrenia patients avoid this disorder. The researchers n the latest study have found important differences in brain development during adolescence between those with schizophrenia and siblings who are healthy and do not have this mental disorder. The study showed that the healthy siblings experienced brain abnormalities similar to their schizophrenic siblings, but in the brain of the healthy sibling the brain development normalized and caught up with the development of normal teens without any indication of schizophrenia. Researchers hope that the latest brain imaging results and findings could open up new treatment possibilities. A partnership between researchers from the National Institute of Mental Health in Washington, D.C and the University of Melbourne in Australia made the study possible.
The brain imaging schizophrenia study used magnetic resonance imaging (MRI) technology to map out the brain development and patterns of 109 individuals who developed childhood-onset schizophrenia between the age of 12 and 24 years old. According to University of Melbourne electrical engineer and lead researcher Dr. Andrew Zalesky “We’ve looked at the development of brain networks over the adolescent period, from childhood to early adulthood. Abnormalities detected early in the unaffected children normalize by age 16. So why are these brothers and sisters able to overcome the risk? Looking for these biological factors that protect a person from developing schizophrenia opens up a new direction in the search for treatments.” According to Melbourne Neuropsychiatry Centre at the University of Melbourne Dr. Christos Pantelis, a co-author of the recent research study, “New generation medications can help young patients manage their symptoms, but can have significant side effects. Our work has the potential to open up avenues towards earlier intervention with fewer side-effects that improve a child’s resilience to becoming ill. This is an interesting new direction, as it suggests the search for targeted psychiatric treatments for schizophrenia and psychosis requires following young people over time.”
Rehab Articles

Is an addiction to sexting becoming a big problem in North America? A new study shows that sexting is more common than what was previously thought, with more than 80% of the people who responded to online surveys admitted that they had engaged in sexting in the last year. The research behind these facts was presented at the 123rd Annual Convention for the American Psychological Association. The research was presented to the convention by Drexel University’s Emily Stasko, MS, MPH. Stasko explained that “Given the possible implications, both positive and negative, for sexual health, it is important to continue investigating the role sexting plays in current romantic and sexual relationships. This research indicates that sexting is a prevalent behavior that adults engage in for a variety of reasons. These findings show a robust relationship between sexting and sexual and relationship satisfaction.”
An addiction to sexting is possible, but this behavior can also play a role in healthy sexual relationships as well. The study involved 870 individuals who were between 18 and 82 years old. Researchers also discovered that many individuals who sexted more often had a higher satisfaction level and rating for their relationship when they were sending these messages to their significant other. When sexting occurs outside of a monogamous relationship it can be harmful to the relationship though. Many experts consider this activity as risky, although many people who engage in sexting view the activity as something fun and harmless. As this activity grows there well be more people who develop an addiction to this risk taking behavior and need treatment.
Rehab Articles
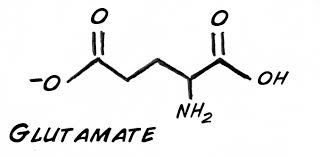
According to University of Illinois at Chicago researchers female depression is often linked to glutamate receptor genes which are overactive. A recent study showed that women who suffer from depression have rates of gene expression which are extremely high, and these abnormal levels occur in the genes which regulate the glutamate system in your brain and body. This is not the only mental or physical health condition that may be caused by glutamate system abnormalities either. In the past these abnormalities have been associated with or linked to epilepsy, Alzheimer’s, autism, schizophrenia, and other disorders. University of Illinois at Chicago pharmacy practice assistant professor Monsheel Sodhi, Ph.D explained the study conclusions and stated “Our data indicate that females with major depression who are at high risk of suicide may have the greatest antidepressant benefit from drugs that act on the glutamate system, such as ketamine.”
The study shows promise for new treatments for female depression which impact the activity of the glutamate receptor gene. According to Dr. Sodhi an overabundance of this neurotransmitter in the brain could explain why women are more likely to attempt suicide when they have female depression. The study results were published in the Molecular Psychiatry journal. The study researchers analyzed brain tissue samples that were recovered postmortem, from both sexes and from individual who both did and did not suffer from mental illness. Many of the individuals whose tissue was analyzed and who were depressed committed suicide. The tissue analysis showed that women who had female depression were more likely to have an overactive glutamate receptor gene.
Rehab Articles
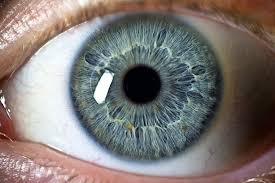
Schizophrenia has been associated with eye movement impairment, and this fact has been known for decades. A new eye test may be able to identify those who are suffering from schizophrenia based on this impairment according to researchers who performed the study. In the study the researchers determines that the eye test accurately identified people who had schizophrenia more than 98% of the time. Lead paper authors for the study, Dr. Philip Benson and Dr. David St. Clair, reported that “It has been known for over a hundred years that individuals with psychotic illnesses have a variety of eye movement abnormalities, but until our study, using a novel battery of tests, no one thought the abnormalities were sensitive enough to be used as potential clinical diagnostic biomarkers.”
The eye test used in the schizophrenia study involved a series of tasks. These tasks included gaze fixation, smooth pursuit, and free viewing. People who have schizophrenia had difficult with the smooth pursuit task, and their eyes had trouble following moving objects. The eye tended to fall behind the object and then to use saccade, a form of REM, to catch back up with the object. The eyes of people with schizophrenia who were shown a picture in the free viewing test differed from the general population because their eyes tracked and followed an abnormal pattern compared with the those who do not have schizophrenia. The fixation tasks of the eye test were also revealing because individuals who have schizophrenia have difficulty holding their gaze steady on a fixed object that does not move.
Rehab Articles

If someone you love struggles with bipolar disorder there are some tips that can make your life and your living situation more productive and easier. 5 great tips that you can use include:
-
Know what bipolar disorder is. Do the necessary research so that you understand what is going on with your loved one and how you can help them. Understanding what your loved one is experiencing will help you and them both.
-
One of the most helpful tips you can learn is to keep notes and pay attention to the symptoms that your loved one is experiencing and displaying. This symptom journal can be very beneficial for medical and mental health professionals, as well as helping you learn what you can expect and how to best manage these symptoms.
-
Communicate openly with your loved on. Ask them what you can do to help them. Don’t be judgmental or make assumptions. Discuss any concerns with the family physician or mental health treatment provider.
-
Don’t let mania catch you off guard. When someone is depressed there are many symptoms common to most individuals, but mania may be displayed differently be each individual who has bipolar disorder. This mental disorder includes lows that can be very low, and highs that have no ceiling. Needing little sleep, having plenty of energy, and being overly optimistic or failing to see that they are on the upswing of bipolar disorder is often noticed by family members. Some may talk excessively, chattering on and on, while others just seem to be in a good mood.
Rehab Articles

A new study by University of Illinois at Chicago (UIC) College of Nursing researchers may have shown the path to predicting binge drinking to some degree through the use of a biomarker. The study involved a biomarker called phosphatidylethanol or Peth, and it is found in much higher amounts in individuals who are more likely to engage in binge drinking. Hopefully this discovery can lead to the ability of predicting who is at risk of binge drinking with a much higher degree of certainty than what is currently possible. According to University of Illinois at Chicago College of Nursing professor and biobehavioral health science department head Mariann Piano, Ph.D. “Binge drinking is pervasive on college campuses and among young adults. More alarming, though, is the regularity of binge drinking episodes: one in five students report three or more binge drinking episodes in the prior two weeks.”
Dr. Piano worked with associate professor of physical therapy and co-researcher Shane Phillips, Ph.D. during the biomarker study on predicting binge drinking. The study involved analyzing blood from the participants. Dr. Piano reported that “We discovered a significant correlation between PEth levels in both the whole blood and dried blood samples and the number of times subjects consumed four to five drinks in one sitting within the last 30 days. Using a biomarker of heavy alcohol consumption such as PEth along with self-reporting could provide an objective measure for use in research, screening and treatment of hazardous alcohol use among young adults.” Binge drinking is a pattern of excessive drinking that occurs in a relatively short period of time and causes a blood alcohol content of over 0.08.
Rehab Articles

Two of the top reasons that people become homeless are mental illness and alcohol abuse or other forms of substance abuse, and a new program called Housing First is taking steps to provide a solution. A recent study found that it is possible to reduce alcohol abuse for those with mental illness in the homeless population by providing these individuals with a safe place to live that has no preconditions attached. The Housing First approach does not place stipulations on a place to live, such as seeing mental health professionals or sobriety testing. Instead Housing First places a focus on getting the homeless individual into permanent housing that allows the individual to live independently. Support and additional services are provided as needed but the homeless individual does not have to follow any preconditions in order to have a safe place to call home.
The underlying ideal behind the Housing First initiative in order to fight alcohol abuse and mental illness among the homeless is that people will be able to move forward and will have a better life if they have stable housing and a more predictable living situation. The study involved 378 people who were all homeless, and who were all diagnosed with some form of mental illness. All of the study participants were from Toronto, Canada. Those who took part in the Housing First initiative saw a drop in alcohol abuse of more than 50%, and this decrease occurred in spite of the fact that the homeless were not forced to stay sober or to follow any other preconditions in order to avoid becoming homeless again.
Rehab Articles

A recent study by University of Houston researchers has identified a connection between alcohol problems, low self esteem, and jealousy. The study found that individuals who rely on their personal romantic relationship for a sense of self esteem typically use alcohol when they experience jealousy. The study and research results have been published in the Addictive Behaviors journal. This is the very first study that identifies a definite connection between relationship dependent self esteem, romantic jealousy, and alcohol problems. The researchers believe that people who have a higher risk of alcoholism can be better identified when the link between these 3 different factors are understood. When this process is fully understood it could lead to better treatment methods for alcohol addiction.
Dr. Angelo DiBello, lead study author of the research on alcohol problems, jealousy, and self esteem, explained the study. “We all experience feelings of jealousy to some degree; many people are in relationships that are less than ideal, and use alcohol for different reasons. Romantic jealousy is a shared human experience, but very little work has looked at how it is related to alcohol use, misuse and associated problems. This research helps to highlight the associations between these factors and show how our emotions, thoughts, and behaviors are related in potentially harmful ways. Given how common experiencing jealousy and being in romantic relationships are, this work helps to explain difference associations that may negatively impact an individual’s drinking. I think it is important to understand the role romantic jealousy plays in the larger context of problem behaviors. Ultimately, I hope to use findings like these to support the development of prevention and intervention efforts among individuals who may struggle with alcohol, self-esteem, and relationship issues.”
Rehab Articles
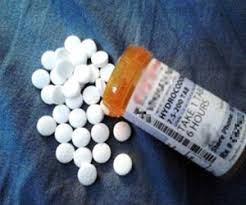
A new research study shows that patients who receive opioid drugs for chronic lower back pain get significantly less pain relief and are more likely to abuse the narcotic pain medications if they also suffer from some form of mental illness as well. According to University of Pittsburgh School of Medicine professor of anesthesiology and psychiatry and study author Ajay Wasan, M.D. “High levels of depression and anxiety are common in patients with chronic lower back pain. Learning that we are able to better predict treatment success or failure by identifying patients with these conditions is significant. This is particularly important for controlled substances such as opioids where, if not prescribed judiciously, patients are exposed to unnecessary risks and a real chance of harm, including addiction or serious side effects.”
The study on chronic back pain, opioid abuse, and mental illness involved 55 participants, and all of these individuals suffered from chronic back pain. Those who had high levels of anxiety or depression saw 50% less back pain relief and improvement, and this group also had 75% more opioid abuse. The group with symptoms of mental illness also saw increased side effects from the pain medications that were used. It is commonly recognized that mental illness, including anxiety and depression, can cause physical pain and other symptoms. Dr Wasan stated “It’s important for physicians to identify psychiatric disorders prior to deciding whether to prescribe opioids for chronic back pain as well as treat these conditions as part of a multimodal treatment plan. Rather than refusing to prescribe opioids, we suggest that these conditions be treated early and preferably before lower back pain becomes chronic. For those prescribed opioids, successful treatment of underlying psychiatric disorders may improve pain relief and reduce the chance of opioid abuse in these patients.”
Rehab Articles
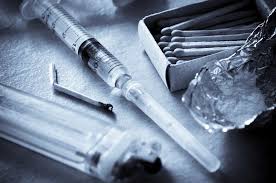
Heroin addiction has reached epidemic rates in the USA and Canada, and there are many challenges when it comes to substance abuse treatment for this problem. There are many different types of programs and facilities, each with specific treatment methods and techniques offered. Insurance coverage and the cost of treatment also play a role in the decisions made. Many insurance companies in the USA will not pay for inpatient care for heroin addiction, although these same insurers will often pay for medical detox and inpatient treatment for alcoholism. The reasoning from many insurers is that heroin addiction is not a medical emergency that can lead to death. Try telling that to someone whose child is at a risk for overdose and death. Every time heroin is used there is a risk of death, and emergency rooms across North America see these cases every day.
Heroin addiction is an insidious problem, and substance abuse treatment is needed but many people can not get help when they seek it at a community program or local facility because of long waiting lists or being unable to afford the cost of an effective inpatient program and treatment regimen. The most effective programs will involve individual counseling, a soothing and peaceful environment, and a wide range of treatment methods and options to choose from. If you or someone you love struggle with a heroin addiction then treatment is critical, continued use of this drug often leads to an early death from an overdose or other medical complications related to heroin use.
Rehab Articles

A new study performed by researchers at prestigious Duke University has identified two brain profiles which are distinct, and one indicates the risk for problem drinking while the other identifies risk for risky sexual behaviors. According to the researchers the scans taken of the study participants showed that brain region functions which were usually complimentary were imbalanced for individuals who had a higher chance of engaging in risky sexual behaviors or problem drinking when the were under stress. The study results could help clinicians accurately predict the risk for these behaviors in young adults in the future although this is not possible yet. The Duke Neurogenetics Study or DNS is an ongoing study which was started in 2010 so that researchers could learn and understand about how brain, environment, and genetic interactions form risky behaviors and predict mental disorders.
The senior study author, for both DNS and the latest study as part of the ongoing process that identified the two distinct brain profiles for problem drinking and risky sexual practices and behaviors, was Duke University psychology and neuroscience professor Ahmad Hariri, Ph.D. According to Dr. Hariri “By knowing the biology that predicts risk, we hope to eventually change the biology or at least meet that biology with other forces to stem the risk. We now have these two distinct profiles of risk that, in general, reflect imbalance in the function of typically complementary brain areas. If you have high activity in both areas, no problem. If you have low activity in both areas, no problem. It’s when they’re out of whack that individuals may have problems with drinking.”
Rehab Articles
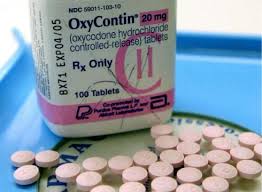
A new study shows that addiction to prescription pain medication is something that a lot of primary care physicians do not understand, even though these same physicians are the top prescribers of these drugs in many areas. The survey showed that a significant number of PCPs do not have a basic understanding of how opioid abuse occurs or about the addiction potential that this class of drugs can have. According to the leader of the study, Johns Hopkins Bloomberg School’s Department of Epidemiology associate professor and Center for Drug Safety and Effectiveness co-director Caleb Alexander, M.D., M.S., “Physicians and patients may mistakenly view these medicines as safe in one form and dangerous in another, but these products are addictive no matter how you take them. If doctors and patients fail to understand this, they may believe opioids are safer than is actually the case and prescribe them more readily than they should.”
The latest prescription pain medication study shows the continuing efforts to understand, identify, and treat opioid addiction in the communities across America. Opiod abuse and addiction has been on the rise, and so has the amount of these drugs on the street. Dr. Alexander continued by saying “Doctors continue to overestimate the effectiveness of prescription pain medications and underestimate their risks, and that’s why we are facing such a public health crisis. Opioids serve an important role in the treatment of some patients. However, our findings highlight the importance of patient and provider education regarding what abuse-deterrent products can and cannot do. When it comes to the opioid epidemic, we must be cautious about overreliance on technological fixes for what is first and foremost a problem of overprescribing.” Alexander also stated “Despite the high levels of support, there are many barriers to implementation and there may be reluctance to translate these changes into real-world practice. But for the sake of making a dent in an epidemic of injuries and deaths, we have to find ways to make changes. Too many lives are at stake to stick with the status quo.”